There is ongoing research into the possibility of a genetic link between attention deficit hyperactivity disorder (ADHD) and the risk of developing Alzheimer’s disease later in life. While there is some evidence to suggest a link, it is important to note that the relationship between these two conditions is complex and not fully understood.
A genetic predisposition to attention deficit/hyperactivity disorder (ADHD) can predict cognitive decline and Alzheimer’s disease later in life, according to a study published today in the journal Molecular Psychiatry by researchers at the University of Pittsburgh School of Medicine.
Although recent large epidemiological studies have suggested a link between ADHD and Alzheimer’s disease, this is the first study to link ADHD genetic risk to the risk of developing late-onset Alzheimer’s disease.
“This study emphasizes what many in the field are already discussing: the impact of ADHD can be seen throughout the lifespan, and it may be linked to neurodegenerative conditions like Alzheimer’s,” said lead author Douglas Leffa, M.D., Ph.D., a psychiatry resident at UPMC.
Tharick Pascoal, M.D., Ph.D., senior author and assistant professor of psychiatry at Pitt, added, “With new treatments becoming available at earlier stages of Alzheimer’s progression, it is important to determine risk factors to help better identify patients who are likely to progress to severe disease.”
This study emphasizes what many in the field are already discussing: the impact of ADHD can be seen throughout the lifespan, and it may be linked to neurodegenerative conditions like Alzheimer’s.
Douglas Leffa
Individuals with ADHD report feeling restless and impulsive and having difficulty maintaining their attention, which leads to a reduction in the quality of their social, school, or work lives, according to the Centers for Disease Control and Prevention. For a long time, ADHD was thought to be a childhood condition that people outgrew once they reached adulthood. ADHD is now recognized as a childhood disorder that can persist into adulthood. ADHD symptoms in adults may be more varied and subtle than in children and adolescents, and it can be especially difficult to diagnose in older adults.
ADHD, like many other behavioral disorders, has a genetic component. However, no single gene determines whether or not its carrier will develop ADHD. Rather, a combination of small genetic changes determines that risk.
Researchers used a previously developed tool called ADHD polygenic risk score, or ADHD-PRS, which represents the combined genetic likelihood of developing the disorder when the entire genome sequence is considered. Because large-scale studies that follow patients with ADHD diagnosed in childhood into old age are scarce, the researchers were forced to work with an incomplete set of data. Rather than relying on clinical diagnosis, they used genetic predisposition to ADHD in their study cohort.
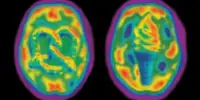
To conduct the study, researchers used a database of 212 adults without cognitive impairments, such as predisposition to other Alzheimer’s related mental health impairments such as dementia, at baseline. The database included brain scans, baseline amyloid and tau levels measured on PET scans and in the cerebrospinal fluid, and results of regular cognitive assessments over the course of six consecutive years. Crucially, researchers also had access to those patients’ genome sequences.
Researchers were able to show that a higher ADHD-PRS can predict subsequent cognitive deterioration and the development of Alzheimer’s brain pathophysiology in the elderly who were previously not cognitively impaired by calculating each patient’s individual ADHD-PRS and matching it with that patient’s signs of Alzheimer’s disease.
While the study findings are intriguing and suggest that the link between ADHD-PRS and Alzheimer’s should be investigated further, the researchers warn against overgeneralizing their findings and urge families to remain informed but calm. Because the database demographic was limited to patients who were white and had more than 16 years of education on average, more work is needed to extend the findings’ applicability beyond a small segment of the American public.
Furthermore, more research is needed to determine whether ADHD interventions can influence the risk of Alzheimer’s disease in the future. Because of the nature of longitudinal studies, a definitive answer may take several decades, though the team is already working to recruit more participants from underrepresented backgrounds and begin follow-up testing.
“Right now, we’re working on new studies to assess ADHD more robustly and enroll childhood ADHD patient cohorts so we can track biomarkers of Alzheimer’s disease over time,” Pascoal said. “These studies take a long time to complete, but they are important for our understanding of multifactorial neurological diseases and how they affect cognitive impairments.”