COVID-19 has long been suspected of causing infertility in men who take it, according to scientists. These new findings reveal that COVID-19 changes the amounts of fertility-related proteins in males, potentially producing long-term reproductive health impacts and problems in male survivors.
Many people who recover from COVID-19 have long-term symptoms including brain fog or heart difficulties. There is growing evidence that the virus can potentially impact fertility. Researchers have now examined protein levels in the sperm of males who have recovered from COVID-19, according to a study published in ACS Omega. According to the researchers, the pilot study reveals that even mild or moderate sickness can alter the amounts of proteins related to male reproductive function.
Although SARS-CoV-2 primarily affects the respiratory system, the virus and the body’s response to it cause harm to other tissues as well. COVID-19 infection has been linked to lower male fertility, and the virus has been found in male reproductive organs. Firuza and Rajesh Parikh of Jaslok Hospital, as well as Sanjeeva Srivastava of the Indian Institute of Technology and colleagues, wondered if COVID-19 infection could have long-term effects on the male reproductive system. To find this, scientists chose to evaluate protein levels in the sperm of healthy men and those who had previously had mild or moderate COVID-19 instances.
The scientists examined sperm samples from 10 healthy men and 17 individuals who had just recovered from COVID-19. There was no prior history of infertility among the men, who ranged in age from 20 to 45. The recovered males had considerably lower sperm count and motility, as well as fewer normally shaped sperm, than men who had not been exposed to COVID-19.
The scientists examined sperm samples from 10 healthy men and 17 individuals who had just recovered from COVID-19. There was no prior history of infertility among the men, who ranged in age from 20 to 45. The researchers discovered that the recovered males had considerably lower sperm count and motility, as well as fewer normally shaped sperm, than men who had not been exposed to COVID-19.
When the researchers used liquid chromatography-tandem mass spectrometry to study semen proteins, they discovered 27 proteins at greater levels and 21 proteins at lower levels in COVID-19-recovered men compared to the control group. Many of the proteins were shown to be involved in reproductive function. Two of the fertility-related proteins, semenogelin 1 and prosaposin, were present at less than half their levels in the COVID-19-recovered group’s sperm compared to the controls’ sperm. According to the researchers, these findings show that SARS-CoV-2 has direct or indirect impacts on male reproductive health that last after recovery.
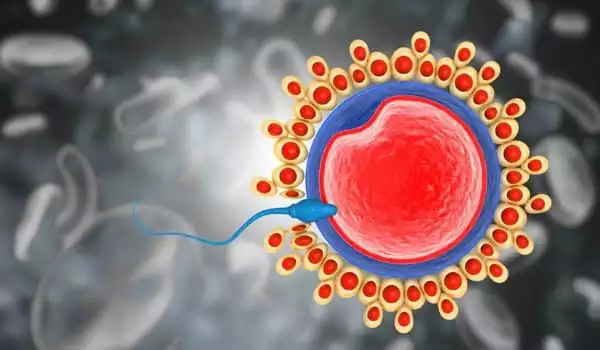
For SARS-CoV-2 to gain entry into a human body and begin to replicate, it needs to bind to something called an ACE2 receptor, a protein found on the surface of cells in the mouth, lungs, heart, and other areas throughout the body. Among all the tissues in the body, the male testis shows nearly the highest level of ACE2 mRNA expression, causing researchers to worry that it could be a target for viral invasion and damage.
They note that the research could provide light on the pathophysiology of human reproduction in recovered men. They do, however, recommend that larger trials be conducted to confirm these findings and that a control group of men who have recently recovered from other flu-like diseases be included to ensure that the findings are specific to COVID-19.
One of the most pervasive and harmful fallacies circulated online is that the COVID-19 vaccine can induce infertility. While that notion has been debunked, the virus’s negative reproductive impact is now well recognized.
Since the beginning of the pandemic, researchers have been tracking the disease’s harmful impact on male fertility. The investigation was accelerated after it was discovered that the virus affects male patients more severely than female patients, presumably due to its mode of transmission. The authors gratefully thank the financial support from Jaslok Hospital.