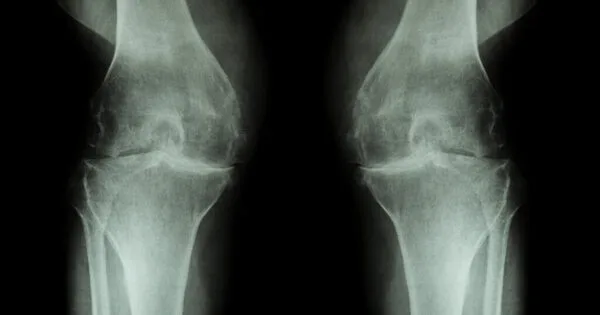
Cartilage is a type of connective tissue that is important for the function of joints, and the ability to generate new cartilage cells could potentially lead to new treatments for conditions such as osteoarthritis, which is characterized by the loss of cartilage in joints. It would be interesting to know more about the specific mechanism that was discovered and what potential applications it could have.
350 million people worldwide are affected by cartilage degeneration and injuries. These conditions cause patients to experience increasing pain and discomfort over time. However, an exciting breakthrough in tissue regeneration research promises significant relief. The study, led by The Forsyth Institute faculty, suggests a new method for producing cartilage cells, which has huge implications in regenerative medicine for future cartilage injuries and degeneration treatments.
As any weekend warrior knows, cartilage injuries to joints such as the knees, shoulders, and hips can be excruciatingly painful and incapacitating. Furthermore, conditions that cause cartilage degeneration, such as arthritis and temporomandibular joint disorder (TMJ), affect 350 million people worldwide and cost the US public health system more than $303 billion annually. These conditions cause patients to experience increasing pain and discomfort over time.
An exciting study led by faculty at The Forsyth Institute, on the other hand, suggests new strategies for making cartilage cells, which could have huge implications in regenerative medicine for future cartilage injuries and degeneration treatments. In a paper titled “GATA3 mediates nonclassical β-catenin signaling in skeletal cell fate determination and ectopic chondrogenesis,” co-first authors Takamitsu Maruyama and Daigaku Hasegawa, as well as senior author Wei Hsu, describe two groundbreaking discoveries, one of which is a new understanding of a multifaced protein known as β-catenin.
The goal of this study was to figure out how to regenerate cartilage. We wanted to figure out how to control cell fate and cause the somatic cell to become cartilage rather than bone.
Dr. Maruyama
Dr. Hsu is a senior scientist at the Forsyth Institute and a Harvard University Professor of Developmental Biology. He is also a member of the Harvard Stem Cell Institute’s affiliate faculty. Swiss scientists Tomas Valenta and Konrad Basler, as well as Canadian scientists Jody Haigh and Maxime Bouchard, were also involved in the research. The research was published in the most recent issue of Science Advances.
“The goal of this study was to figure out how to regenerate cartilage,” explained Dr. Maruyama of Forsyth. “We wanted to figure out how to control cell fate and cause the somatic cell to become cartilage rather than bone.”
Previously, it was thought that the Wnt signal transduction pathway was the determinant of whether a cell became bone or cartilage. The master factor transducing the Wnt signals is β-catenin. The basis for this belief was the result that when β-catenin was disrupted, the bone became cartilage.
However, β-catenin also acts as a cell adhesion molecule to facilitate cell-cell interaction — the original function identified prior to the discovery of its role in Wnt signaling. “We know that this molecule is important for cell fate determination, but the mechanism remained open to study,” said Dr. Hsu.
The team tested what would happen when β-catenin was only partially impaired for signaling, finding that, in that case, the cells were unable to form bone or cartilage. After these tests, the scientists concluded that Wnt signaling is a determinant for bone formation, but that it isn’t sufficient for cartilage generation.
“We wanted to know what the factor was for cell fate determination,” said Dr. Maruyama. “What reprograms a cell to become cartilage if it isn’t Wnt signaling?”
GATA 3, an alternative action of -catenin responsible for skeletal cell fate switching, was discovered in response to this question. GATA3 is a single gene regulator that activates the expression of cartilage-specific genes in cells.
“GATA3 binds to the genome sequences required for reprogramming,” explained Dr. Wei Hsu. GATA3 is a game changer because it has the potential to transform any somatic cell into a cartilage-forming cell, similar to how four stem cell factors can be used to generate embryonic stem cell-like cells known as induced pluripotent stem cells (iPSC).”
Controlling cell fate in this way allows researchers to direct a cell to become bone, cartilage, or fat, which has huge implications for developing new treatments for the 1 in 4 people who suffer from cartilage injuries and degeneration. There is no treatment that can regenerate cartilage at the moment, and current treatments are incapable of improving joint function.