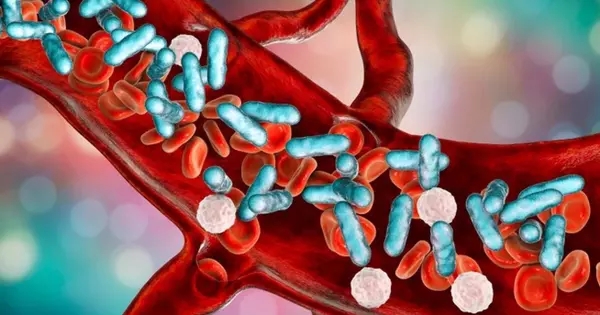
Research on blood clotting has provided promising insights into the treatment and management of sepsis. Sepsis is a life-threatening condition that occurs when the body’s response to infection becomes dysregulated, leading to widespread inflammation and organ dysfunction. Blood clotting plays a critical role in sepsis, as both excessive clotting and impaired clotting can contribute to its progression.
Researchers from the University of Birmingham, UK, who identified a novel mechanism for platelet activation in pathogenic blood clotting (thrombosis) are now turning their attention to sepsis.
Identified by Associate Professor Julie Rayes and Dr Martina Colicchia from the Birmingham Platelet Group, and described in a recent paper in Blood, this previously unknown axis comprises platelet receptor glycoprotein I alpha (GPIb?), and an anti-microbial protein S100A8/A9, which is released from activated immune cells.
The mechanism is not blocked by classical anti-platelet drugs currently used to treat arterial thrombosis, and is distinct from the well-described ‘clotting cascade’ that limits blood loss following injury.
When clots form at the site of a vascular injury, two main populations of platelets are seen. Highly activated and aggregated platelets are found at the clot’s core, while procoagulant platelets are found in the shell around the core and help to generate fibrin, which helps to stabilize the clot.
Julie Rayes
“When clots form at the site of a vascular injury, two main populations of platelets are seen,” Dr Rayes explains. Highly activated and aggregated platelets are found at the clot’s core, while procoagulant platelets are found in the shell around the core and help to generate fibrin, which helps to stabilize the clot.”
“The S100A8/A9-GPIb? axis does not induce platelet aggregation, but it does induce procoagulant platelet formation and accelerates fibrin activation and thrombosis.” This axis may be more important in disease states where innate immune cells and platelets play a critical role in clotting.”
High levels of S100A8/A9 are seen in the blood in thrombo-inflammatory diseases including myocardial infarction (MI), deep vein thrombosis (DVT) and infections such as COVID-19 and sepsis, and their presence correlates with thrombotic complications and worse outcomes for patients.
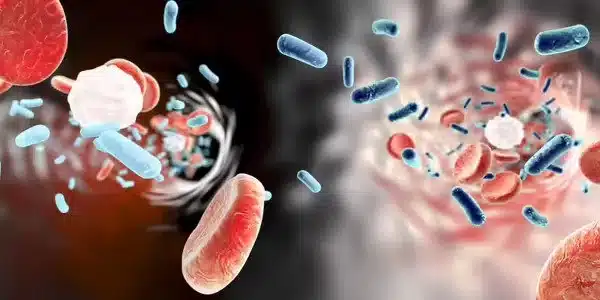
The researchers believe this novel mechanism may be relevant in thrombosis observed under chronic inflammatory conditions and acute infections and believe that the interaction of S100A8/A9 with multiple receptors* makes it an interesting target to limit both clotting and inflammation during sepsis.
“Thrombosis is a major complication during infection,” Dr. Rayes explained, “so drugs that target pathogenic clotting while maintaining vascular integrity and the normal clotting process (haemostasis) are required.” We hope to limit inflammation and thrombosis during infection by selectively targeting S100A8/A9, a key pathogenic inflammatory and thrombotic molecule.”
The University of Birmingham Enterprise has filed a patent application covering the targeting of the S100A8/A9-GPIb? axis in the treatment and prevention of thrombosis in chronic inflammatory and thrombotic diseases, and is now seeking commercial development or licensing partners.
While more research on blood clotting in sepsis is needed, these findings have the potential to improve sepsis management. Researchers hope to mitigate the negative effects of excessive clotting while preventing complications associated with impaired clotting by targeting and modulating clotting processes. These advancements may eventually lead to better outcomes for septic patients.