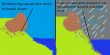
Superbugs, or antibiotic-resistant bacteria, have become a major worldwide health concern as a result of antibiotic abuse and misuse, resulting in the evolution of bacteria that are no longer sensitive to typical antibiotic treatments. Scientists are continually looking for novel ways to develop antibiotics that can overcome resistance mechanisms and treat diseases caused by resistant bacteria.
A decades-long scientific journey at Duke University has yielded a novel antibiotic method for combating gram-negative bacteria such as Salmonella, Pseudomonas, and E. coli, which cause many urinary tract infections (UTIs). In animal testing, the synthesized chemical works quickly and is long-lasting.
It operates by interfering with a bacterium’s ability to produce its exterior lipid layer, or “skin.”
“If you disrupt the synthesis of the bacterial outer membrane, the bacteria cannot survive without it,” said lead researcher Pei Zhou, a biochemistry professor at Duke University. “Our compound is very good and very potent.”
If you disrupt the synthesis of the bacterial outer membrane, the bacteria cannot survive without it. Our compound is very good and very potent.
Pei Zhou
LPC-233 is a tiny chemical that has been shown to disrupt outer membrane lipid production in every gram-negative bacterium tested. Co-authors from the University of Lille in France tested it against a collection of 285 bacterial types, including several that were highly resistant to market antibiotics, and it killed them all.
And it works fast. “LPC-233 can reduce bacterial viability by 100,000-fold within four hours,” Zhou said.
The molecule is also strong enough to make it all the way to the urinary system following oral delivery, making it a potentially useful tool in the fight against persistent urinary tract infections (UTIs). According to the findings, tests at high doses of the substance revealed “exceedingly low rates of spontaneous resistance mutations in these bacteria,” according to a research published in Science Translational Medicine.
The chemical proved successful in animal experiments when given orally, intravenously, or injected into the abdomen. In one experiment, mice were given a potentially deadly dose of multidrug-resistant germs, yet the novel substance saved them.
The search for this compound took decades because of the specificity and safety required of the synthetic molecule.
Zhou credits his late colleague, former Duke Biochemistry Chair Christian Raetz, for starting the search decades ago. “He spent his entire career working on this pathway,” Zhou said. “Dr. Raetz proposed a conceptual blueprint for this pathway in the 1980s, and it took him over two decades to identify all of the players,” Zhou said.
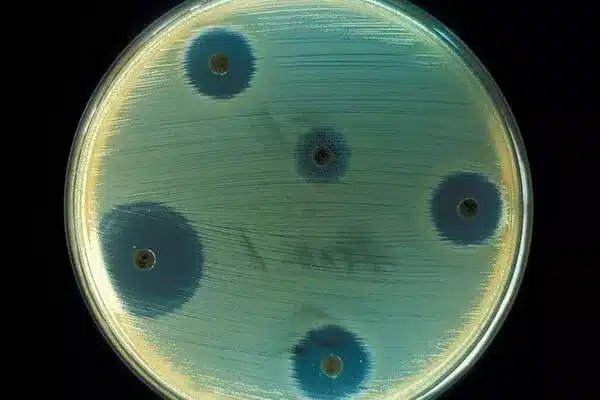
The new drug’s target is an enzyme called LpxC, which is the second enzyme in the “Raetz pathway” and is required for gram-negative bacteria to produce outer membrane lipid.
Raetz became the chairman of biochemistry at Duke in 1993, after his work on this pathway at Merck & Co. failed to produce a viable clinical candidate. The Merck antibiotic was effective against E. coli, but it was not commercially feasible, therefore the pharmaceutical company abandoned it.
“He actually recruited me to Duke to work on this enzyme, initially just from the structural biology perspective,” said Zhou, who joined Duke in 2001.
Zhou and Raetz had solved the structure of the LpxC enzyme and revealed molecular details of a few potential inhibitors. “We realized that we could tweak the compound to make it better,” Zhou said. Since then, Zhou has been working with his colleague, Duke Chemistry professor Eric Toone, to make more potent LpxC inhibitors.
The first human trial of LpxC inhibitors had failed because of cardiovascular toxicity. The focus of the Duke group’s subsequent work was to avoid cardiovascular effects while maintaining the potency of the compound.
They worked on more than 200 different versions of the enzyme inhibitor, always searching for better safety and more potency. Other compounds worked to varying degrees, but compound number 233 was the winner.
LPC-233 fits a binding spot on the LpxC enzyme and prevents it from doing its work. “It fits in the right way to inhibit formation of the lipid,” Zhou said. “We’re jamming the system.”
Zhou explained that the chemical operates in a remarkable two-step manner, which adds to its durability. After binding to LpxC, the enzyme-inhibitor complex changes shape slightly to become a more stable combination.
The inhibitor binding in this more stable compound has a longer lifetime than the bacterium. “We believe that contributes to potency because it has a semi-permanent effect on the enzyme,” he explained. “Even after the unbound drug has been metabolized by the body, the enzyme is still inhibited due to the extremely slow inhibitor dissociation process,” Zhou explained.
There are multiple patents being filed on the series of compounds, and Toone and Zhou have co-founded a company called Valanbio Therapeutics, Inc. which will be looking for partners to bring LPC-233 through phase 1 clinical trials to assess safety and efficacy in humans.