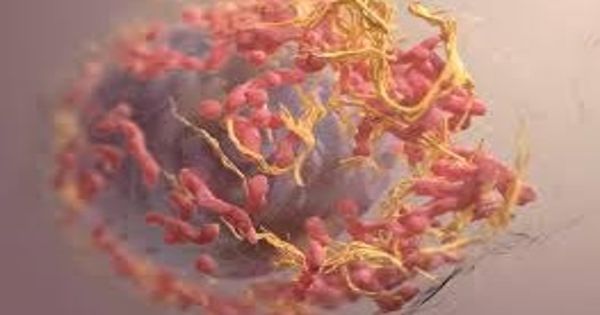
The vaccine induces a long-lasting anti-tumor response in melanoma patients. Four years after patients with melanoma received a customized cancer vaccine, the vaccine-engineered immune response remains strong and successful in holding cancer cells under the balance, researchers at the Dana-Farber Cancer Center, Brigham and Women’s Hospital, and the Large Institute of MIT and Harvard reported in a new review.
Melanomas are cancers that arise from melanocytes that appear to exhibit early metastases that are secondary to the lack of cellular conformity in the primary tumor, resulting in elevated mortality rates. Cancer-specific active immunotherapy is an experimental method of therapy that stimulates the immune system to detect antigens on the surface of cancer cells. Human melanomas are malignant tumors produced by melanocytes. As an advanced form of skin cancer, melanoma is a significant cause of morbidity and death.
A personalized cancer vaccine produced a long-lasting anti-tumor response in patients with melanoma. Four years after vaccination, all the patients were alive, with immune system cells active not only against tumor cells with those proteins but also spread to other proteins in those tumor cells.
The results, published online today by Nature Medicine, indicate the continued effectiveness of the vaccine-generated immune response, known as NeoVax, by targeting particular proteins in the tumor cells of each patient. Researchers observed that, almost four years after vaccination, immune system cells in patients were involved not only against tumor cells with these distinctive proteins, but also against other proteins found in tumor cells in these patients.
“These findings demonstrate that a personal neoantigen vaccine can stimulate a durable immune response in patients with melanoma,” says study co-leader Catherine J. Wu, MD, of Dana-Farber, Brigham and Women’s Hospital (BWH), and the Broad Institute. “We found evidence that the initial, targeted immune response has broadened over the years to provide patients with continued protection from the disease.”
Melanomas are some of the most recognized immunogenic tumors and are thus a successful model method for immunocompromised vaccine therapy. The study included eight patients who had undergone advanced melanoma surgery but were deemed at high risk of recurrence. A total of 18 weeks after surgery, NeoVax was treated in Phase 1 clinical trial. The vaccine is made from pieces of protein called epitopes that peek from the cell surface and act as signals to the immune system.
NeoVax epitopes come from neoantigens—abnormal tumor cell proteins that warn that the cell is cancerous and should be killed. Since neoantigens are present only in tumor cells, they activate an immune response that prevents normal cells from attacking. In order to make NeoVax, the sequence of DNA in a patient’s tumor is screened to identify the main epitopes within the tumor cell neoantigens. The epitopes act as targets for T cells, which contribute to an attack on cancer by the immune system. When a patient is infected with NeoVax, the epitopes are used to draw an immune system response against any melanoma cells that display them.
In the new study, researchers found that a median of four years after NeoVax, all eight patients were alive, six of which exhibited no symptoms of active disease. When they studied the T cells of the patients—the immune system cells that triggered vaccine action—they found evidence that the cells not only “remembered” their original target epitopes but also extended their repertoire to recognize other melanoma-related epitopes.
Two of the patients whose cancer had spread to their lungs had administered an immune checkpoint inhibitor, a medication that loosens some of the constraints on the immune response to cancer. In these two patients, the researchers found evidence that T cells had made their way to the tumor tissue, where they could be the most lethal to the melanoma cells.
“We found evidence of everything we look for in a strong, sustained immune response,” says Patrick A. Ott, MD, Ph.D., Dana-Farber, Brigham and Women’s Hospital (BWH) and Broad Institute, who co-led the Wu report. “T cells tended to destroy particular melanoma cells and maintained the memory of the epitopes they originally reacted to. T cells were activated to kill tumor cells and, importantly, diversified to attack melanoma epitopes not included in the original vaccine.
“The long-term persistence and expansion of the melanoma-targeting T cells is a strong indication that personal neoantigen peptide vaccines can help control metastatic tumors, particularly when combined with immune checkpoint inhibition.”