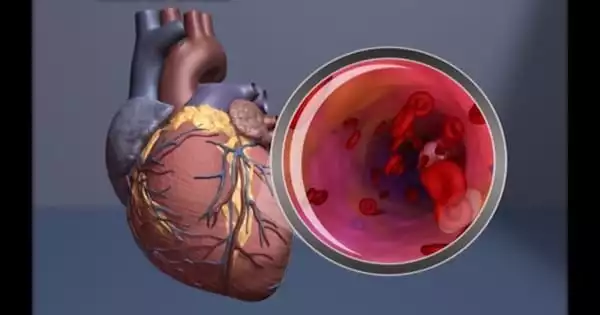
A study of nearly 600,000 persons in the United States discovered that people with bipolar disorder, schizophrenia, or schizoaffective disorder had up to double the projected cardiovascular risk levels as those without such disorders, even at younger ages. According to new research published in the Journal of the American Heart Association, an open access, peer-reviewed journal of the American Heart Association, the study focused on adults diagnosed with one of those three serious mental illnesses who were not hospitalized or living in a mental health treatment center and estimated their 10-year and 30-year cardiovascular risk.
Researchers believe that earlier detection and care of key cardiovascular risk factors, such as obesity, smoking, diabetes, and high blood pressure, in young adults with serious mental illnesses may lower the risk of heart disease and improve outcomes.
“Previous research has shown that people diagnosed with a serious mental illness die 10-20 years earlier than the general population, and their leading cause of death is heart disease,” said study lead author Rebecca C. Rossom, M.D., M.S., a senior research investigator in behavioral health at the Center for Chronic Care Innovation at HealthPartners Institute in Minneapolis, Minnesota. “Our study compared overall heart disease risk in adults with and without major mental illness by focusing on the role of cardiovascular risk factors such as blood pressure, cholesterol, blood sugar, body mass index, and smoking status.”
Our study compared overall heart disease risk in adults with and without major mental illness by focusing on the role of cardiovascular risk factors such as blood pressure, cholesterol, blood sugar, body mass index, and smoking status.
Rebecca C. Rossom
According to the researchers, this is the first study to look at predicted 30-year (lifetime) cardiovascular risk in a large sample of adult outpatients diagnosed with bipolar disorder, schizophrenia, or schizoaffective disorder – three major mental diseases that are unique to this study. According to Rossom, many earlier studies of cardiovascular risk in people with major mental illness have only included people who were hospitalized, and they tend to have more severe mental disease and frailer health than outpatients. This study, on the other hand, contained a large sample of non-hospitalized U.S. individuals.
Bipolar disorder (previously known as manic-depressive disease or manic depression) is a mental condition that produces extraordinary swings in mood, energy, activity levels, focus, and ability to carry out daily duties, according to the National Institute of Mental Health. Schizophrenia can lead to hallucinations, delusions, and slurred speech. People suffering with schizophrenia may appear to have lost contact with reality, which can be extremely distressing for the individual, their family, and friends. Schizophrenia symptoms can be chronic and incapacitating. The Diagnostic and Statistical Manual of Mental Disorders defines schizoaffective disorder as a continuous period of illness characterized by a major mood episode (manic or depressed) in addition to fitting schizophrenia criteria.
This study looked at health data from over 600,000 persons between the ages of 18 and 75 who went to a primary care clinic in Minnesota or Wisconsin between January 2016 and September 2018. A diagnosis of significant mental illness was given to about 2% of adults, or approximately 11,000 people. Seventy percent were diagnosed with bipolar illness, 18% with schizoaffective disorder, and 12% with schizophrenia. People with major mental diseases were more likely to be younger, female, self-identify as Black, Native American, Alaskan, or of various races, and have Medicaid or Medicare coverage than their counterparts who had not been diagnosed with one of the three serious mental illnesses.
Prediction models using defined metrics were used to analyze cardiovascular risk variables and forecast the likelihood of a heart attack, stroke, or death from cardiovascular causes. The American College of Cardiology/American Heart Association’s atherosclerotic cardiovascular risk scoring tool was used to determine 10-year risk in persons aged 40 to 75. The Framingham Risk Score was used to calculate 30-year cardiovascular risk in persons aged 18 to 59.
Researchers found:
- Those in the study who had one of the significant mental diseases examined had a 10-year cardiovascular risk level of 9.5 percent, compared to 8 percent for adults who did not have a mental condition.
- Individuals with one of the three serious mental illnesses had a significantly higher estimated 30-year risk of cardiovascular disease – 25% compared to 11% of those without a serious mental illness.
- The elevated risk of heart disease was seen even in young persons (ages 18-34) suffering from a significant mental condition.
- Within the subtypes of each of the three serious mental illnesses studied in this study, in analyses adjusted for age, gender, race, ethnicity, and insurance coverage, people with bipolar disorder had the highest 10-year cardiovascular risk compared to those with schizophrenia or schizoaffective disorder, and people with schizoaffective disorder had the highest 30-year cardiovascular risk when compared to the other two groups.
- Smoking and body mass index (BMI) accounted for the majority of the risk factors contributing to cardiovascular disease in those with a serious mental illness: those with a serious mental illness were three times more likely to be current smokers (36%) than peers without a serious mental illness (12%), and 50 percent of those with a serious mental illness met the criteria for obesity compared to 36 percent of people without a serious mental illness.
- Diabetes (Type 1 or Type 2) was diagnosed at twice the rate in patients with major mental illnesses as in people without serious mental disease (14 percent vs. 7 percent , respectively).
- High blood pressure was seen in 15% of adults with a significant mental illness compared to 13% of those without a serious mental illness.
“Even at younger ages, those with major mental illness had a higher risk of heart disease than their peers,” Rossom said. “This underscores the need of addressing cardiovascular risk factors for these individuals as early as feasible.” “Interventions to reduce the risk of heart disease in these persons are most successful when began at a younger age.”
“We encourage health care systems and doctors to adopt 30-year cardiovascular risk estimates for young persons with major mental illness, which can be used as early as age 18,” she said. “At the moment, estimations of 10-year heart disease risk are most commonly employed, and they cannot be used until people are at least 40 years old, which is too late to begin treating heart disease risk in persons with major mental illness.”