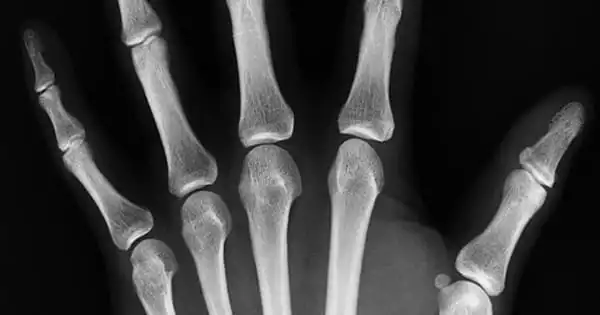
Prednisone and other drugs, as well as aging, can weaken our bones, and scientists working to prevent both have some of the first evidence that the best target may not be the logical one. According to Dr. Meghan E. McGee-Lawrence, biomedical engineer in the Department of Cellular Biology and Anatomy at the Medical College of Georgia, the mineralocorticoid receptor, better known for its role in blood pressure regulation, is a key factor in bone health in aging bone.
And, according to McGee-Lawrence, corresponding author of the study published in the Journal of Bone and Mineral Research, drugs that block the receptor, such as the hypertension medications spironolactone and eplerenone, may help protect bone cells.
Prednisone and other glucocorticoids are well-known for their roles in reducing inflammation and suppressing the immune response, which is why they work so well for conditions such as irritable bowel syndrome and arthritis. However, they, like aging, can disrupt the healthy, ongoing dynamic of bone formation and destruction.
Our natural glucocorticoid levels rise with age, and bone has more glucocorticoid receptors than mineralocorticoid receptors when we are young. Glucocorticoids can induce stem cells to produce bone-forming osteoblasts, but they also cause those osteoblasts to store more fat, and too much fat in the bone, like anywhere else on our body, is probably not good and typically correlates with bone loss, according to McGee-Lawrence. As a result, reducing the influence of glucocorticoid receptors seemed like a logical way to protect bone.
We’re curious about what causes bone cells to change which receptors they express and how they respond to these. However, aging brings about a slew of changes. Because we know that inflammation changes with age, there are many different cues that could cause these things to change.
Dr. Meghan E. McGee-Lawrence
The MCG researchers were already surprised to discover that removing functional glucocorticoid receptors did not protect against bone loss in younger mice fed calorie-restricted diets. In fact, there was an increase in fat accumulation in the bone marrow, which worsened the osteoporosis.
They were looking at the impact of endogenous glucocorticoids in an aging model this time, and they discovered that when the glucocorticoid receptor was blocked, older mice experienced more fat accumulation in the bone marrow and worsening bone disease.
They also discovered that the mice had less muscle mass, moved less than normal mice, and had higher blood pressure. Another surprise was that many of the problems were reversed when they used drugs to inhibit the mineralocorticoid receptor.
“The only way we’ve found to get rid of that lipid storage by osteoblasts was to use drugs to inhibit the mineralocorticoid receptor,” she says, and fortunately, because of the receptors’ clear role in blood pressure, there are already drugs that do just that.
“I think what it means is that we can’t just think about signaling through one receptor if we want to understand what these stress hormones, these endogenous glucocorticoids, are doing,” McGee-Lawrence says. She believes mineralocorticoid receptors may be a better target for older bone.
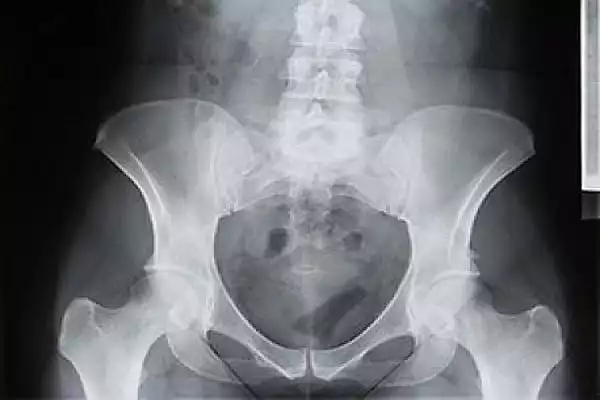
“We thought knocking out the glucocorticoid receptor would improve things, but it actually made things worse,” McGee-Lawrence says. “We believe the mineralocorticoid receptor could explain a lot of what’s wrong with aging bone.”
Both receptors are members of the steroid receptor family, and it is thought that mineralocorticoid receptors have equal affinity for mineralocorticoids and glucocorticoids. She speculates that the signaling pathways in young and old people may differ.
McGee-Lawrence and her colleagues have already discovered that the expression of mineralocorticoid receptors in bone increases, potentially significantly, with age. They have preliminary mixed results on whether glucocorticoid receptors decline with age and are learning more about what happens with both receptor levels as well as the role of mineralocorticoid receptors in bone, particularly aging bone.
“We’re curious about what causes bone cells to change which receptors they express and how they respond to these,” she says. “However, aging brings about a slew of changes. Because we know that inflammation changes with age, there are many different cues that could cause these things to change.”
The whole-body impact they saw from their receptor manipulation, such as higher blood pressure from deleting the glucocorticoid receptor, she says, is evidence of bone’s importance as an endocrine organ.
“By changing glucocorticoid signaling in the bone, we are seeing changes in the fat, muscle, adrenal glands, and physical activity,” she says, implying that something from the bone is communicating with all of these other body systems, an emerging role of research in her field.
In fact, the increased fat presence in bone marrow found in osteoporosis has led to it being classified as a metabolic bone disease, similar to how obesity, particularly excess weight around the middle, is classified as a metabolic disease. Increased fat in the bone marrow is linked to disuse, such as after a spinal cord injury, a high-fat diet, using glucocorticoids, such as steroids, and aging.
While fat is a ready source of energy for bone cells, too much of it can inhibit bone cell formation. The scientists aren’t sure whether the cells are no longer using fat well or if they are pulling in more fat, or both; they do know that fat accumulating in bone cells corresponds with less bone being made, she emphasizes.
“We’re trying to figure out exactly why these things are going wrong so that we can choose the best treatment strategy,” she says. There is a lot of evidence in people that synthetic glucocorticoids, which we take by pill or injection, can have an effect on bone, creating an unhealthy imbalance between the amount of bone made and the amount broken down.
A focus of MCG research has been examining the bone impact of our endogenous glucocorticoids, which we produce, a less-explored area. McGee-Lawrence and her colleagues have been studying bone-forming osteoblasts for years, which, like most cells, do not function optimally as we age. However, it is possible that even synthetic glucocorticoids work through these alternative receptors to damage the bone, which means that attempting to prevent their damage may require a different target, she says, noting that the pathway may change as the person ages.
Interestingly, some other tissues known to have a high density of mineralocorticoid receptors inactivate glucocorticoids, which bone cannot do, but she speculates that it compensates by having a low density of mineralocorticoid receptors, at least in youth.
Both glucocorticoids and mineralocorticoids are produced by the adrenal gland, and their production becomes less well-regulated as we age.