Sexual contact has been shown to transmit more than 30 different bacteria, viruses, and parasites. Eight of these pathogens have been linked to the highest rates of sexually transmitted disease. Syphilis, gonorrhoea, chlamydia, and trichomoniasis are the only four of these eight infections that are currently curable. The other four are incurable viral infections: hepatitis B, herpes simplex virus (HSV or herpes), HIV, and human papillomavirus (HPV). Treatment can reduce or modify symptoms or diseases caused by incurable viral infections.
Sexual contact, including vaginal, anal, and oral sex, is the most common way STIs spread. Some STIs can also be transmitted non-sexually, such as through blood or blood products. Many STIs, such as syphilis, hepatitis B, HIV, chlamydia, gonorrhea, herpes, and HPV, can be passed from mother to child during pregnancy and childbirth.
An STI can exist in the absence of obvious disease symptoms. Vaginal discharge, urethral discharge or burning in men, genital ulcers, and abdominal pain are all common symptoms of STIs.
We show how skin vaccination can generate protective CD8 T-cells that are recruited to the genital tissues and could be used as a vaccination strategy for sexually transmitted infections in a new study (STIs).
Professor Linda Klavinskis
Researchers from King’s College London demonstrated how skin vaccination can generate protective CD8 T-cells that are recruited to genital tissues and could be used as a vaccination strategy for sexually transmitted infections in a study published in Nature Communications (STIs).
Understanding how to attract specialized immune cells, known as CD8 T-cells, to take up residence in the part of the body where the virus first enters the body is one of the challenges in developing vaccines for STIs such as HIV or herpes simplex virus. Instead of waiting for immune cells in the blood to enter the tissues, which takes time, these cells must be present, armed, and ready to provide an immediate protective immune defense.
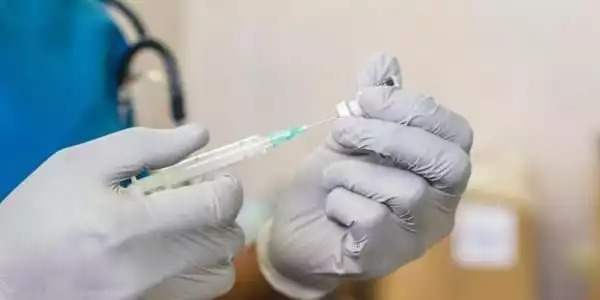
Prior to this study, it was thought that vaccines should ideally be delivered directly to the body surface (e.g., female genital tissue) where the infection may begin, so that the immune system can generate these CD8 T-cells, travel back to the vaccination site, and eliminate any future virus encountered. Delivering vaccines directly to female genital tissue, on the other hand, is neither patient-friendly nor efficient.
The King’s team has discovered that their vaccination strategy marshals a platoon of immune cells called innate lymphoid cells (ILC1) and monocytes in the genital tissues to collaborate and release chemicals (chemokines) to summon the CD8 T-cells generated by the vaccine.
This study expands on the team’s previous work to develop skin vaccination techniques that use a dissolvable’microneedle’ vaccine patch that, when placed against the skin, dissolves and releases the vaccine without the need for a hypodermic needle injection and generates immune responses.
“This study highlights how specialized groups of ‘innate’ immune cells in distant tissues can be harnessed to attract protective CD8 T-cells, arming the body’s frontline tissues against infection,” said lead author Professor Linda Klavinskis of King’s College London.
“We now need to confirm these findings with other types of vaccines than the one used in the study to see if skin vaccination activates a common pathway.” If proven, this could significantly improve the efficacy of vaccines against sexually transmitted infections.”
Sexually transmitted infections (STIs) have a significant impact on sexual and reproductive health around the world. Every day, over 1 million STIs are purchased. The World Health Organization estimated 376 million new infections with one of four STIs in 2016: chlamydia (127 million), gonorrhoea (87 million), syphilis (6.3 million), and trichomoniasis (156 million). More than 500 million people are infected with genital HSV (herpes), and an estimated 300 million women are infected with HPV, the primary cause of cervical cancer. Globally, an estimated 240 million people have chronic hepatitis B. Vaccination can protect against both HPV and hepatitis B infections.