Researchers discovered that three different autism risk genes affect similar elements of neuron development and neuron types, although acting via distinct chemical processes. Furthermore, a person’s distinct genomic background fine-tuned the impact of the genes. The research was carried out with the use of microscopic 3D replicas, or ‘organoids,’ of the human cerebral cortex, the region of the brain responsible for cognition, perception, and language. The findings contribute to our understanding of autism spectrum disorder and represent a first step in finding treatments for the ailment.
Autism spectrum disease has been linked to hundreds of different genes, however it is unclear how these disparate genetic changes result in a comparable pathology in patients. Researchers at Harvard University and the Broad Institute of MIT and Harvard have discovered that three different autism risk genes affect the same components of neural formation and the same types of neurons in the growing human brain. The researchers discovered identical overall abnormalities for each risk gene by evaluating them in miniature 3D models of the human brain called “brain organoids,” despite the fact that each one worked through unique underlying chemical pathways.
The results, published in the journal Nature, give researchers a better understanding of autism spectrum disorder and are a first step toward finding treatments for the condition.
“Much research is being done in the field to see whether there are any commonalities among the many risk genes connected with autism. Finding such similar traits may point to common targets for wide therapeutic intervention, regardless of disease genetic origin. Our findings reveal that many disease mutations do, in fact, converge on harming the same cells and developmental processes, albeit via different methods. These findings encourage further research into therapeutic approaches aimed at modulating shared dysfunctional brain properties “Paola Arlotta, the Golub Family Professor of Stem Cell and Regenerative Biology at Harvard University and an institute member in the Stanley Center for Psychiatric Research at the Broad Institute, is the study’s senior author.
We presented a method for producing organoids with the unique capacity to develop reproducibly in 2019. They create the same types of cells and in the same order as the developing human cerebral cortex.
Silvia Velasco
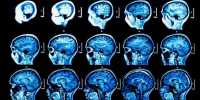
The Arlotta lab studies organoid models of the human cerebral cortex, which is responsible for cognition, perception, and language. The models begin as stem cells and develop into a 3D tissue including many of the cell types found in the cortex, including neurons that can fire and connect into circuits.
“We presented a method for producing organoids with the unique capacity to develop reproducibly in 2019. They create the same types of cells and in the same order as the developing human cerebral cortex” Silvia Velasco, a senior postdoctoral scholar in the Arlotta lab and a co-lead author on the current study, explained. “It’s a dream come true to realize that organoids may now be used to learn something unexpected and novel about a disease as complex as autism.”
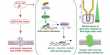
The researchers created organoids with a mutation in one of three autism susceptibility genes known as SUV420H1, ARID1B, and CHD8. “We chose to start with three genes that could have a wide range of functions. They don’t have a clear role that might readily explain what happens in autism spectrum disorder, so we were curious to see if these genes were doing anything similar “Bruna Paulsen, a postdoctoral fellow in the Arlotta group and co-lead author, explained her findings.
The organoids were grown over several months by the researchers, closely mimicking the stages of development of the human cerebral cortex. The organoids were then analyzed using several technologies, including single-cell RNA sequencing and single-cell ATAC-sequencing to measure changes and regulation in gene expression caused by each disease mutation; proteomics to measure responses in proteins; and calcium imaging to see if molecular changes were reflected in abnormal activity of neurons and their networks.

“This study was only possible because of the collaboration of several labs that came together, each with their own expertise, to attack a complex problem from multiple angles,” said co-author Joshua Levin, an institute scientist at the Broad Institute’s Stanley Center and the Klarman Cell Observatory.
The researchers discovered that the risk genes all had a similar effect on neurons, either accelerating or slowing down brain development. In other words, the neurons formed at an inopportune period. Furthermore, the risk genes all impacted the same two populations of neurons, an inhibitory type known as GABAergic neurons and an excitatory type known as deep-layer excitatory projection neurons. This indicated that certain cells may be special targets in autism.
“The cortex is built in a highly choreographed manner: each type of neuron develops at a precise time and begins to connect extremely early. If certain cells grow too early or too late compared to when they should, you may be altering the way circuits are ultimately wired “Martina Pigoni, a former postdoctoral fellow in the Arlotta lab and co-lead author, shared her thoughts.
In addition to assessing different risk genes, the researchers created organoids using stem cells from various donors. “Our goal was to examine how changes in the organoids might be influenced by an individual’s unique genetic background,” said Amanda Kedaigle, a computational biologist at the Arlotta lab and co-lead author.
The general abnormalities in neural development were similar in organoids generated from different donors, although the severity differed across people. The impacts of the risk genes were fine-tuned by the rest of the donor genome.
“It’s perplexing how the same autism risk gene variants may cause such disparities in clinical presentations in patients. We discovered that different human genomic contexts can modulate the manifestation of disease phenotypes in organoids, implying that in the future, we may be able to use organoids to disentangle these distinct genetic contributions and gain a better understanding of this complex pathology” According to Arlotta.
“Genetic research has been extremely successful in finding genetic changes linked to autism spectrum disorders and other neurodevelopmental diseases. The difficult next step on the path to discovering new treatments is determining exactly what these mutations do to the developing brain “said Steven Hyman, a Harvard University Distinguished Service Professor of Stem Cell and Regenerative Biology, the director of the Stanley Center at the Broad, and a Broad Institute core member.
“By identifying the changes in brain circuits that occur when genetic variants are present, we can take a tentative next step toward better diagnosis and find new pathways for therapeutic research.”