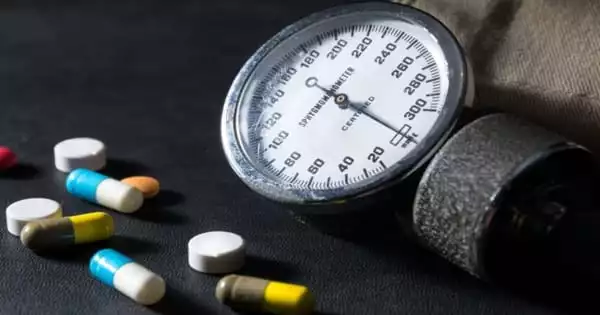
High blood pressure during pregnancy remains a major cause of maternal and fetal pregnancy-related complications and death, and it increases women’s short- and long-term risks for cardiovascular disease. Emerging data from clinical trials and observational research support the benefits and safety of blood pressure treatment during pregnancy. Continued investigation is critical to determine which blood pressure levels, during- and post-pregnancy, both for starting therapy and as treatment goals, are beneficial for the mother and safe and beneficial for the fetus.
Treatment for high blood pressure during pregnancy appears safe for many women and may reduce maternal risk for severe hypertension without increasing fetal and neonatal risks, according to a new American Heart Association scientific statement published in the Association’s journal Hypertension.
A scientific statement is an expert analysis of current research that may inform future clinical practice guidelines. In this statement, “Hypertension in Pregnancy: Diagnosis, Blood Pressure Goals, and Pharmacotherapy,” experts in obstetrics and gynecology, maternal-fetal medicine, cardiology, nephrology, hypertension, and internal medicine reviewed and analyzed quality studies on high blood pressure during pregnancy, including gestational hypertension and preeclampsia/eclampsia.
According to the most recent American Heart Association statistics, hypertension during pregnancy is the second leading cause of maternal death worldwide, with a systolic pressure (the top number in a blood pressure reading) of 140 mm Hg or higher. Severe cases are linked to an increased risk of cardiovascular complications for mothers immediately or shortly after delivery, as well as for years afterward. Pregnancy hypertension increased the risk of complications for the child, such as preterm delivery, small for gestational age, and low birth weight. Globally, rates of hypertension during pregnancy are rising, and data show that it disproportionately affects women of diverse racial and ethnic backgrounds in the United States, particularly those who are Black, American Indian, or Alaskan Native.
For many years, the benefits of blood pressure medication for pregnant women were unknown. There were also concerns about fetal well-being from antihypertensive medication exposure.
Vesna D. Garovic
The goals of treatment during pregnancy include preventing severe hypertension and avoiding premature birth to give the fetus time to mature before birth.
“For many years, the benefits of blood pressure medication for pregnant women were unknown. There were also concerns about fetal well-being from antihypertensive medication exposure” Vesna D. Garovic, M.D., Ph.D., a professor of medicine and chair of the division of nephrology and hypertension with a joint appointment in the department of obstetrics and gynecology at Mayo Clinic in Rochester, Minnesota, chaired the statement writing group.
“It is reassuring to see emerging evidence that treating high blood pressure during pregnancy is safe and effective and may be beneficial at lower thresholds than previously thought, based on our comprehensive review of the existing literature. We now have a current statement focused on hypertension during pregnancy to help guide optimal treatment and future research.”
According to the statement, the United States has one of the highest rates of hypertensive-related maternal mortality among high-income countries. Cardiovascular disease, which includes stroke and heart failure, now accounts for up to half of all maternal deaths in the United States, and hospitalizations for pregnancy-related stroke increased by more than 60% between 1994 and 2011. According to the American Heart Association, preeclampsia, which occurs when hypertension during pregnancy is accompanied by signs of liver or kidney problems such as protein in the urine, affects 5% to 7% of pregnancies and is responsible for more than 70,000 maternal deaths and 500,000 fetal deaths worldwide each year.

“Given the rising number of cases of hypertension during pregnancy, as well as hypertension-related complications,” Garovic said, “the problem has become a public health crisis, especially among women from racially and ethnically diverse backgrounds.”
While the general population’s definition of hypertension is 130/80 mm Hg, according to the 2017 American College of Cardiology (ACC)/American Heart Association (AHA) Guideline for the Prevention, Detection, Evaluation, and Management of High Blood Pressure in Adults, most guidelines around the world define hypertension during pregnancy as 140/90 mm Hg.
Because of concerns about how medications may affect the fetus, there is no agreement on when to begin hypertension treatment during pregnancy. Several health advocacy organizations recommend starting treatment when blood pressure levels during pregnancy range from 140/90 mm Hg (Canadian guidelines) to 160/110 mm Hg (U.S. guidelines).
The new statement cites evidence that blood pressure-lowering therapy for pregnancy hypertension reduces the incidence of severe hypertension significantly. More research is needed to determine how much treating hypertension at a lower threshold may reduce serious hypertensive complications, such as organ damage and hypertensive emergencies. The authors of the statement write that reducing severe hypertension may be especially important in communities that lack the resources and expertise to respond to hypertension emergencies.
“Future research should look into whether lowering the threshold for treating hypertension during pregnancy could allow for safe and timely blood pressure control and avoid a rushed delivery due to uncontrolled hypertension,” Garovic said.
According to the most recent research, treating hypertension during pregnancy with blood pressure-lowering medication does not appear to have a negative impact on fetal growth or development. Preventing hypertension during pregnancy benefits maternal health both during and after childbirth. It is well known that those who have hypertension during pregnancy are more likely to develop chronic hypertension after pregnancy than those who have normal blood pressure during pregnancy.
The statement reinforces recent research that suggests lifestyle changes before and during pregnancy have the potential to improve maternal and fetal outcomes:
- Dietary changes before and during pregnancy can limit weight gain and improve pregnancy outcomes.
- Exercise during pregnancy may reduce gestational hypertension risk by about 30% and preeclampsia risk by about 40%.
The statement also highlights these areas of concern:
- There is emerging evidence that hypertension after delivery (postpartum) may be associated with significant maternal health problems.
- The current science suggests physicians should individualize treatment decisions, considering risk factors and patient preferences.
- The care of women with hypertension during pregnancy is often complex, and a multispecialty team of health care professionals may be beneficial.
“Future clinical trials will be required to answer questions about when to start treatment for high blood pressure during pregnancy,” Garovic said. “In addition, close collaboration between the American Heart Association and the American College of Obstetricians and Gynecologists will be critical in optimizing diagnosis and treatment of hypertension during pregnancy, as well as improving immediate and long-term outcomes for many women who develop hypertension during pregnancy.”