Working hours that differ from a person’s natural body clock are linked to an increased risk of cardiovascular disease, according to research presented at ESC Preventive Cardiology 2021, an online scientific congress of the European Society of Cardiology (ESC).
“Our study discovered that every hour the work schedule was out of sync with an employee’s body clock, the risk of heart disease increased,” said study author Dr. Sara Gamboa Madeira of the University of Lisbon in Portugal.
Working hours that deviate from an individual’s natural body clock are associated with greater cardiovascular risk, according to recent research.
At least 20% of European employees work unusual hours or shifts2, and growing scientific evidence links these to negative cardiovascular outcomes. 3 Several explanations have been advanced, including sleep disruption and unhealthy behaviors. The role of circadian misalignment, which is the difference between the “social clock” (e.g., work schedules) and the individual “biological clock,” was examined in this study.
Dr. Gamboa Madeira elaborated: “We all have an internal biological clock that ranges from morning types (larks) who feel alert and productive in the early morning and sleepy in the evening to late types (owls) who feel the opposite – with the majority of the population falling somewhere in between. Circadian misalignment occurs when there is a mismatch between what your body desires (e.g., falling asleep at 10 p.m.) and what your social obligations require (e.g., working until midnight).”
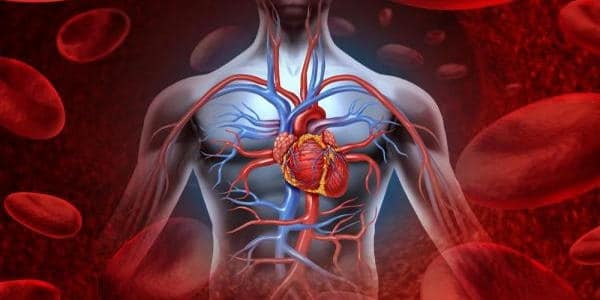
The study included 301 blue-collar workers who were all performing manual picking activity in a retail company’s distribution warehouses in Portugal. Staff always worked early morning (6 a.m.-3 p.m.), late evening (3 p.m.-midnight), or night shifts (9 p.m.-6 a.m.). Participants filled out a questionnaire about sociodemographic factors (age, gender, education), occupational factors (work schedule, seniority), and lifestyle factors, and their blood pressure and cholesterol levels were measured.
The Munich ChronoType Questionnaire was used to determine sleep duration and the internal biological clock of each individual (also called chronotype). It was also used to calculate the amount of circadian misalignment (the difference between an individual’s biological clock and working hours), also known as social jetlag. Participants were divided into three groups based on the number of hours of social jetlag they experienced: 2 hours or less, 2-4 hours, and 4 hours or more.
To calculate relative cardiovascular risk, the researchers used the European relative risk SCORE chart, which incorporates smoking, blood pressure, and cholesterol. The relative risk scale runs from 1 (nonsmoker with normal blood pressure and cholesterol) to 12. (smoker with very high blood pressure and cholesterol). A relative risk of 3 or higher was considered “high cardiovascular risk” in this study. The researchers then looked into the link between social jetlag and an increased risk of cardiovascular disease.
The average age of the participants was 33 years, with men accounting for 56% of the total. Just over half of those polled (51%) were smokers, 49 percent had high cholesterol, and 10% had hypertension. One-fifth (20%) were classified as having a high cardiovascular risk. On workdays, 40% slept for a short period of time (6 hours or less). The average amount of social jetlag was nearly two hours. The majority of workers (59%) experienced social jetlag in 2 hours or less, while 33% experienced it in 2-4 hours and 8% experienced it in 4 hours or more.
A higher level of social jetlag was associated with an increased risk of being in the high cardiovascular risk group. Even after controlling for sociodemographic, occupational, lifestyle, and sleep characteristics, as well as body mass index, the odds of being classified as high cardiovascular risk increased by 31% for each additional hour of social jetlag.
According to Dr. Gamboa Madeira: “These findings add to the growing body of evidence that circadian misalignment may explain, at least in part, the link discovered between shift work and negative health outcomes. The findings imply that employees with unusual work schedules may require closer monitoring for heart health. Longitudinal research is needed to determine whether late chronotypes cope better with late/night shifts and earlier chronotypes cope better with early morning schedules, both psychologically and physiologically.”