Luring a virus into a trap may not be a viable strategy as viruses are not sentient beings and do not have the ability to make conscious decisions. Viruses are tiny infectious agents that can only replicate by infecting a host cell and using the host’s cellular machinery to make copies of themselves.
Viruses such as influenza A and Ebola infiltrate human cells in a series of steps. Using electron tomography and computer simulations, research teams from Heidelberg University and Heidelberg University Hospital investigated the final stages of viral penetration in an interdisciplinary approach.
They were able to determine how the immune system fights off the virus in the case of influenza A by using a small protein. They discovered that in order for an Ebola virus infection to take hold, a specific protein structure must be disassembled. These processes rely heavily on so-called fusion pores, which allow the viral genome to enter the host cell. If they are prevented from forming, the virus is also prevented from spreading. The Heidelberg scientists describe previously unknown mechanisms, which might lead to new approaches to prevent infections.
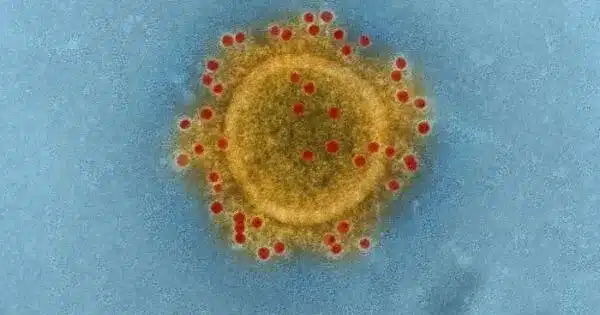
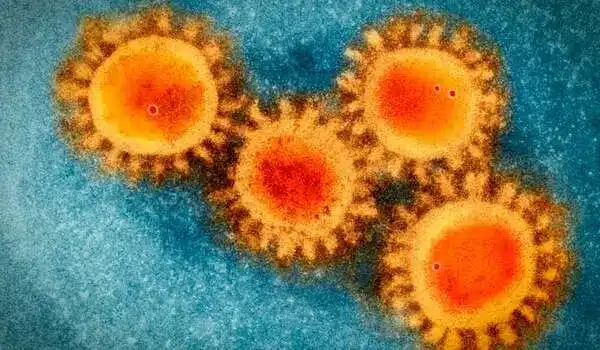
Many viruses that infect humans have a lipid membrane that contains glycoproteins that can bind to human cells. These are the spike proteins that bind to epithelial cells in the nose and lungs in viruses like influenza A that enter through the respiratory tract. The highly infectious Ebola virus, on the other hand, spreads through direct contact with infected bodily fluids and can infiltrate a wide range of cell types. After invading human cells, these viruses must open a fusion pore between the virus membrane and the host membrane in order to release their genome and spread.
This specialized protein can effectively prevent viruses such as influenza A, SARS-CoV-2, and Ebola from penetrating, but the underlying mechanisms were unknown. The viruses are literally captured in a lipid trap. Our research indicates that they are ultimately destroyed.
Dr. Petr Chlanda
To combat the virus, the human immune system attempts, in stages, to prevent the formation of the fusion pore. Infected cells detect the presence of the foreign genome and send a signal to uninfected cells in the form of an interferon molecule. This signal causes uninfected cells to produce interferon-induced transmembrane protein 3 (IFITM3), a small cellular protein.
“This specialized protein can effectively prevent viruses such as influenza A, SARS-CoV-2, and Ebola from penetrating, but the underlying mechanisms were unknown,” states virologist Dr. Petr Chlanda, whose working group belongs to the BioQuant Center of Heidelberg University and the Center for Integrative Infectious Disease Research of Heidelberg University Hospital. The researchers were now able to demonstrate that for influenza A viruses, IFITM3 selectively sorts the lipids in the membrane locally. This prevents the fusion pores from forming. “The viruses are literally captured in a lipid trap. Our research indicates that they are ultimately destroyed,” explains Dr Chlanda.
Dr. Chlanda and his colleagues used equipment from Ruperto Carola’s Cryo-Electron Microscopy Network to examine the structural details of viruses. Using computer simulations, the research groups led by Prof. Dr. Ulrich Schwarz of the BioQuant-Center and the Institute for Theoretical Physics, as well as Prof. Dr. Walter Nickel of the Heidelberg University Biochemistry Center, predicted this process in an interdisciplinary approach. The researchers believe that in the context of antiviral therapy, it is possible to develop lipid-sorting peptides that insert themselves into the virus membrane, rendering the viruses incapable of membrane fusion. “Such peptides could be used in a nasal spray, for example,” Petr Chlanda says.
In a second study, the Heidelberg researchers looked into the Ebola virus’s penetration and fusion. A flexible protein envelope known as the VP40 matrix protein layer determines the virus’s filamentous morphology. “It has always puzzled us how this long virus could penetrate the cell, fuse with the membrane, and release its genome,” Dr. Chlanda explains. The researchers discovered that this virus protein envelope disassembles at a low pH, i.e. in an acidic environment, using structural analysis of infected but inactive cells provided by collaborators from the Friedrich Loeffler Institute in Greifswald.
This step is crucial for the formation of fusion pores, as further computer simulations by Profs. Schwarz and Nickel demonstrated. The electrostatic interactions of the VP40 matrix with the membrane are weakened during this process, lowering the energy barrier of pore formation. According to the findings of the Heidelberg basic research, preventing the disassembly of this layer is one way to keep Ebola viruses from forming fusion pores. The Ebola virus, like the influenza A virus, would then be lured into a trap from which it could not escape.